Retinal Vein Occlusion: Causes, symptoms, and treatment options
Retinal Vein Occlusion (RVO) is one of the most common vascular disorders affecting the retina. It is a leading cause of sudden, painless vision loss, particularly in adults over 50 years of age. Although the condition may sound alarming, early diagnosis and timely treatment can significantly improve outcomes and help preserve vision.
This guide is designed to help individuals and their families understand the causes of RVO, how it is diagnosed, and the available treatment options.
Retinal Vein Occlusion: What It Means & What to Do
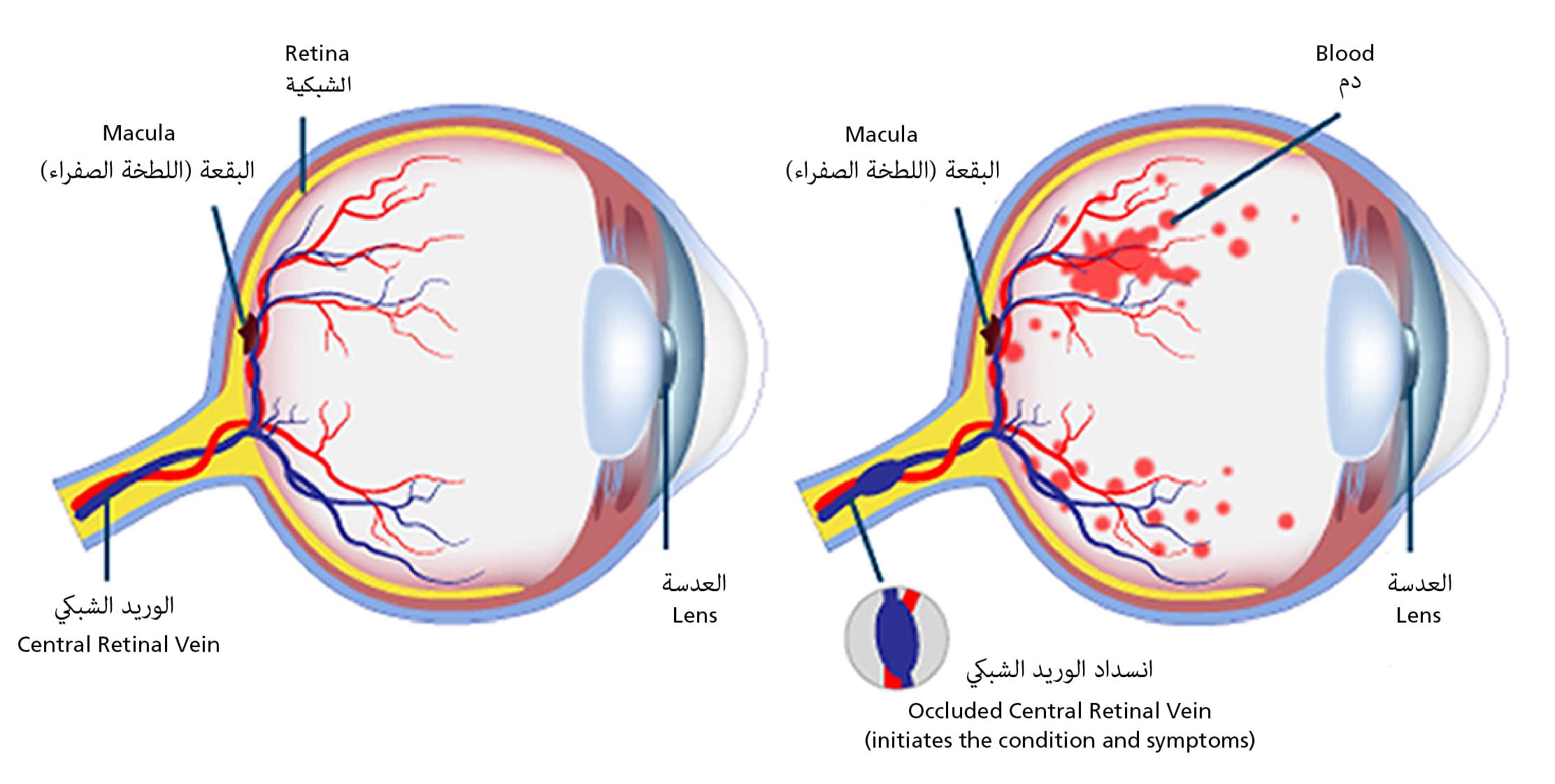
Retinal Vein Occlusion occurs when one of the veins responsible for draining blood from the retina becomes blocked. The retina is the light-sensitive tissue located at the back of the eye, which is essential for processing visual information. When blood flow is interrupted, fluid may accumulate (known as macular oedema), leading to swelling, bleeding, and in severe cases, permanent vision loss.
This blockage usually affects one eye and can happen suddenly. The severity and treatment approach depend on the location and extent of the blockage.
Types of Retinal Vein Occlusion
There are two main types of Retinal Vein Occlusion, each with distinct characteristics:
- Central Retinal Vein Occlusion (CRVO): This occurs when the central vein responsible for draining the entire retina is blocked. CRVO is often associated with more significant vision impairment and may lead to complications such as macular oedema, abnormal blood vessel growth (neovascularisation), or increased eye pressure (neovascular glaucoma).
- Branch Retinal Vein Occlusion (BRVO): BRVO involves a blockage in one of the smaller branches of the central retinal vein. It tends to cause more localised and less severe vision loss compared to CRVO.
Causes Retinal Vein Occlusion
RVO is often linked to changes in blood vessels and underlying health conditions. Common risk factors include:
- Hypertension (high blood pressure): Chronic high blood pressure can damage the retinal vessels, increasing the risk of occlusion.
- Diabetes: Diabetes can lead to changes in blood vessels throughout the body, including those in the eye.
- Cardiovascular Disease: Conditions that affect circulation, such as atherosclerosis (hardening of the arteries), increase the risk of retinal vein blockage.
- Glaucoma: Elevated eye pressure can contribute to vein compression.
- Blood Clotting Disorders: Rare clotting conditions or thickened blood can contribute to blockages in the retina.
- High cholesterol (Hyperlipidaemia): Elevated lipid levels contribute to blood vessel narrowing and clot formation.
In some cases, RVO may occur without a known cause, particularly in younger individuals. This is why a comprehensive evaluation is essential.
Symptoms of Retinal Vein Occlusion
The most common symptom is a sudden, painless loss of vision in one eye. Other symptoms may include:
- Blurred or distorted central vision
- Partial or complete loss of vision in one eye
- Dark spots or floaters in the visual field
- A general dimming of vision
- Sudden onset of visual disturbances, such as dark patches or floaters
It is important to note that RVO is usually not associated with eye pain or redness, which distinguishes it from other acute eye conditions.
Diagnosing Retinal Vein Occlusion
Diagnosis is made during a comprehensive eye examination by an ophthalmologist. This may include:
- Dilated Fundus Examination: Using eye drops to dilate the pupil, the doctor examines the retina for signs of haemorrhage, swelling, or abnormal blood vessels.
- Optical Coherence Tomography (OCT): This non-invasive imaging test provides high-resolution images of the retina to detect macular swelling and monitor treatment response.
- Fluorescein Angiography: A special dye is used to identify areas of poor circulation or leakage from blood vessels.
- Visual acuity test and intraocular pressure (IOP) measurement: To assess baseline vision and rule out contributing factors, such as glaucoma.
These tests help differentiate between CRVO and BRVO, guiding the development of appropriate treatment plans.
Treatment options for Retinal Vein Occlusion
Although there is no direct way to unblock the vein, treatment focuses on reducing swelling, preserving vision, and managing the underlying causes.
Ocular treatments of Retinal Vein Occlusion
- Observation: In some cases, particularly with mild BRVO not affecting the central retina (macula), the eye may be monitored closely without immediate intervention
- Intravitreal Injections: These are the most common treatments for macular oedema resulting from RVO:
- Anti-VEGF (Vascular Endothelial Growth Factor) agents, such as ranibizumab or aflibercept, help reduce fluid buildup and prevent abnormal blood vessel growth.
- Steroid injections may be used if anti-VEGF is not effective or suitable.
Treatment is usually given over several months and personalised to each patient’s progress.
- Laser Photocoagulation: This may be used to treat areas of poor retinal circulation (non-perfusion) or to control abnormal blood vessel growth, especially in BRVO cases.
Systemic treatments of Retinal Vein Occlusion
Managing the underlying medical conditions is crucial in preventing further eye damage and reducing the risk of RVO recurrence. This includes:
- Controlling blood pressure
- Managing blood sugar levels in diabetic patients
- Treating high cholesterol
- Lifestyle changes such as quitting smoking, maintaining a healthy weight, and regular exercise
In some cases, your ophthalmologist may collaborate with a general physician or cardiologist for a coordinated care approach.
What Is the outlook for patients with Retinal Vein Oclusion?
The visual outcome depends on several factors, including the location of the blockage, whether the macula is involved, and the timing of treatment initiation.
With appropriate care, many people regain stable or improved vision. However, long-term monitoring may be needed. If left untreated, complications such as neovascular glaucoma, retinal detachment, or persistent swelling can occur.
Living with Retinal Vein Occlusion
A diagnosis of RVO can feel overwhelming, but with support and proper management, many individuals adjust well. It is important to:
- Attend all follow-up appointments
- Adhere to medication schedules
- Monitor for any sudden changes in vision
- Take steps to maintain cardiovascular health
- Seek emotional support or low-vision rehabilitation if vision loss persists
When to see a Retina specialist in Dubai for Retinal Vein Occlusion?
If you experience sudden changes in your vision, especially in one eye, or have known risk factors such as diabetes or high blood pressure, it is essential to seek prompt medical care. Early diagnosis and treatment can be vision-saving.
At Moorfields Eye Hospital Dubai, our retina specialists provide expert care for all forms of Retinal Vein Occlusion, utilising advanced diagnostic imaging and evidence-based treatment plans tailored to each patient.
Frequently Asked Questions about Retinal Vein Occlusion
Is Retinal Vein Occlusion the same as a stroke in the eye?
While not technically the same, Retinal Vein Occlusion (RVO) is often referred to as an “eye stroke” because it involves a sudden blockage in one of the veins that drain blood from the retina, the light-sensitive tissue at the back of the eye. Much like a stroke in the brain, this blockage can disrupt normal function and lead to lasting damage. However, RVO occurs only in the eye and typically affects one side, whereas cerebral strokes involve brain tissue and may affect a wider range of functions.
Can RVO cause total blindness?
Complete blindness from RVO is rare; however, the condition can lead to significant vision impairment, especially if left untreated promptly. The most severe visual loss typically occurs when the macula, the part of the retina responsible for detailed central vision, is affected. Complications such as macular oedema or abnormal blood vessel growth (neovascularisation) can also contribute to vision loss. Timely diagnosis and ongoing treatment can help protect vision and prevent further deterioration.
Is the condition painful?
RVO is typically painless. Many patients only become aware of it after noticing a sudden change in vision, such as blurriness, dark spots, or partial loss of sight. The absence of pain can make early detection challenging, so it is important to seek immediate medical attention if you notice unexplained vision changes, even if there is no discomfort.
Can I drive if I have RVO?
Whether you can continue to drive depends on the degree of vision loss and its impact on your ability to see clearly, especially at night or in peripheral areas. Your ophthalmologist will assess your visual acuity and field of vision to determine if it is safe for you to drive. In some cases, restrictions may be advised for your safety and the safety of others.
How can I prevent RVO from happening again?
Prevention focuses on controlling the underlying risk factors that contribute to vein occlusion. This includes maintaining healthy blood pressure, managing diabetes and cholesterol levels, quitting smoking, and staying physically active. Regular follow-ups with both your ophthalmologist and primary care physician are vital.
Will I need injections for the rest of my life?
Not necessarily. Some patients respond well to a few initial injections and require less frequent treatments over time, while others may need long-term management to keep swelling under control. Your doctor will monitor your condition and adjust your treatment plan to suit your eye’s response and overall progress.